Nigerian Decentralized Three-tiered Structure
According to the World Health Organization (WHO), the Sub-Saharan region, where Nigeria is located, alone accounts for 11 percent of the world's population and yet bears 24 % of the global disease burden, and commands less than 1% of the global health expenditure. Nigeria falls below the WHO standard of 2.3 health workers per 1000 of population.
The Medical and Dental Council of Nigeria (MDCN) figures show that the doctor to patient ratio is about 1:6500 and that between 2007 and 2011, there was a net loss of 2095 doctors from Nigeria due to emigration. Nigerian healthcare system is, in principle, decentralized into a three-tiered structure with responsibilities at federal, state and local government levels. The local governments manage the local dispensaries (primary healthcare), the State Ministries of Health (SMOH) manage various General Hospitals (secondary healthcare).
The role of Federal Ministries of Health (FMOH) is confined to framing of policies and management of Teaching Hospitals and Federal Medical Centers (tertiary healthcare). Contribute towards the provision of optimal health for all Nigerians in line with existing national health policy. Coordinate the formulation of public health policies and guidelines. Support their implementation and evaluation in Nigeria through health promotion, surveillance, prevention and control of diseases.
Nigeria Health Insurance Scheme

National Health Insurance Scheme (NHIS) launched with great fanfare in May 1990 has not made any impact with poor country wide penetration of less than 4%. There is gross shortage of doctors, nurses and other clinical and non-clinical staff, the important link in the healthcare value chain.
The salaries too are not attractive enough for good talent. 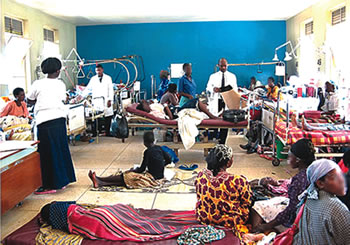 Most of the high end medical equipment and drugs are imported, leading to major losses in revenue.
Most of the high end medical equipment and drugs are imported, leading to major losses in revenue.
The overall healthcare delivery system is therefore highly inefficient and falls much short of the prevailing requirement. Health Insurance as an alternative source of funding is feasible in Nigeria, with potential to secure universal access needed to strengthen existing structures; modify some areas; creative stakeholder engagement; and facilitate rapid programme uptake at State level.
Barriers to Services in the Rural Areas

High cost of medical and surgical services, lack of access and transportation, lack of proper infrastructure, lack of adequate electricity, and lack of qualified providers in the rural areas. Brain drain is therefore a major issue with a large number of doctors, nurses and paramedical staff leaving the Nigerian shores for better opportunities outside, mainly to the United States & Europe.
About 2% of Nigerian doctors and 12% of Nigerian nurses work outside Nigeria. The remaining are then inappropriate skill mix and varying levels of performance across the country.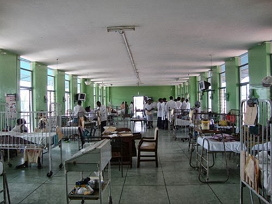 However, often due to scant financial and human resources locally and a lack of interest in delivering preventive programs by foreign, short-term medical mission volunteers, most missions are left treating illnesses rather than preventing them.
However, often due to scant financial and human resources locally and a lack of interest in delivering preventive programs by foreign, short-term medical mission volunteers, most missions are left treating illnesses rather than preventing them.
A properly planned medical/health mission with a long term vision will lead to a lasting impact on the health system.